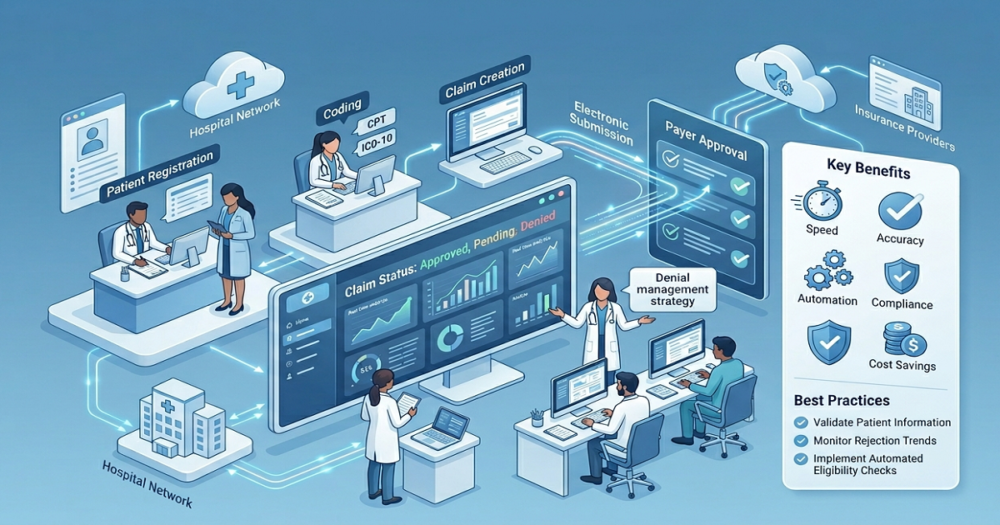
Delays in billing don’t usually start at the payer’s end. They begin earlier: when the claim is still being prepared. A missing field, a wrong format, or a detail that wasn’t verified properly. None of these stops the process immediately, which is why they’re easy to miss.
What happens next is more noticeable. Claims don’t move as expected. Some stay pending longer than usual. Others come back for correction. Over a few weeks, the pattern becomes clearer: payments are slower, and rework is increasing.
That’s where electronic claim submission changes the equation. Not by speeding things up blindly, but by putting checks in place before the claim is sent out.
What Changes When Claims Are Submitted Electronically
At a basic level, it’s about sending claims digitally. But that’s not the part that makes the difference.
The difference is what happens before submission. Instead of pushing a claim forward and waiting to see what comes back, the system reviews it first. Missing data, incorrect codes, and format issues: these are flagged early. That doesn’t eliminate errors completely, but it reduces the number that reach the payer.
In manual workflows, those same issues often show up only after rejection. That’s where time is lost.
How the Workflow Moves in Real Terms
The process itself hasn’t changed. The way it’s handled has.
Patient Details and Eligibility
It starts at intake. If the insurance information isn’t verified properly, the claim is already exposed to risk. Electronic systems can check this in real time, which removes a lot of guesswork.
Coding and Claim Setup
Documentation is converted into code. This step still depends on accuracy. The system doesn’t decide what’s correct; it only checks if something is missing or inconsistent.
Claim Scrubbing
Before the claim goes out, it’s reviewed automatically. If something doesn’t match requirements, it’s flagged. For instance, a missing modifier may not stop the claim immediately, but it can lead to a denial later. Catching it here avoids that cycle.
Clearinghouse Check
The claim passes through a clearinghouse. It performs another round of validation and sends it to the correct payer.
Payer Review
At that stage, it’s in the payer’s hands. They review the details and decide whether to pay it, deny it, or send it back for clarification.
Payment and Follow-Up
Once processed, payments are recorded. Any issues that remain need follow-up. Each step connects to the next. If something is off early, it doesn’t disappear, but it shows up later.
Where the Real Gains Come From
Electronic submission improves outcomes in ways that are easy to measure.
- Claims reach payers faster
- Fewer claims are rejected at the first stage
- Status updates are easier to track
- Teams spend less time correcting basic errors
These are practical improvements. They don’t change how billing works, but they make it more consistent.
What It Doesn’t Fix on Its Own
Switching to electronic submission doesn’t solve everything.
If coding doesn’t match documentation, the claim can still be denied. If patient information is entered incorrectly, the system won’t correct it automatically. If eligibility isn’t checked properly, the issue remains.
In other words, the system reduces technical errors. It doesn’t fix process gaps. That part still depends on how the team works.
Best Practices That Keep Claims Moving
This is where most of the difference shows up. Not in the system itself, but in how it’s used.
Check Information Before Submission
Even with validation in place, incorrect details can slip through. Verifying data early prevents avoidable delays.
Don’t Ignore System Flags
When something is flagged, there’s usually a reason. Skipping it saves time in the moment but adds more work later.
Keep Coding Consistent
The system won’t correct coding decisions. If documentation doesn’t support the code, the claim is still at risk.
Look at Claims Early
Checking status within the first week helps catch issues before they grow.
Fix Patterns, Not Just Claims
If the same rejection appears multiple times, it’s not random. It points to a gap that needs to be corrected at the source.
Where Teams Lose Time Without Noticing
Some delays don’t come from major mistakes. They come from small habits.
- Claims sent without reviewing alerts
- Follow-ups delayed because “it should go through”
- Rejections handled individually instead of identifying patterns
- Processes not updated when payer rules change
None of these stops billing. They just slow it down enough to affect results.
The Role of Clearinghouses
Clearinghouses add another layer of review before the claim reaches the payer.
They check:
- Required fields
- Claim structure
- Routing accuracy
This reduces the chance of immediate rejection. But they don’t check whether the service billed is clinically accurate. That still depends on documentation and coding.
Measuring Whether It’s Working
You don’t need complex reporting to understand performance. A few indicators are enough.
- How many claims are accepted on the first submission
- How many are returned for correction
- How long does it take to receive payment
- Whether the same issues keep appearing
These numbers show whether your electronic claim submission process is improving or just maintaining the same problems.
Keeping It Consistent as Volume Increases
As the workload grows, it becomes tempting to skip steps. That’s usually when errors increase. The better approach is to keep the process simple and repeatable. The same checks, the same flow, every time.
It may feel slower at first, but it prevents rework later.
Conclusion
Electronic claim submission doesn’t change the fundamentals of billing. It changes how consistently those fundamentals are applied.
When claims are checked properly before submission and tracked afterward, delays are reduced, and payments come in with fewer interruptions.
Rapid RCM Solutions works with healthcare practices to strengthen billing workflows, reduce submission errors, and improve reimbursement timelines by making sure the process holds up under real-world conditions.