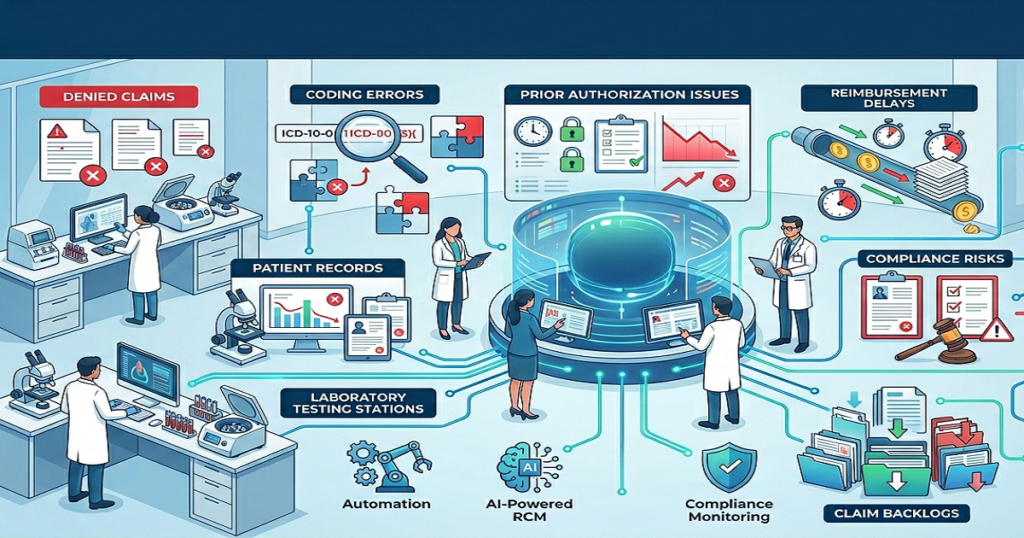
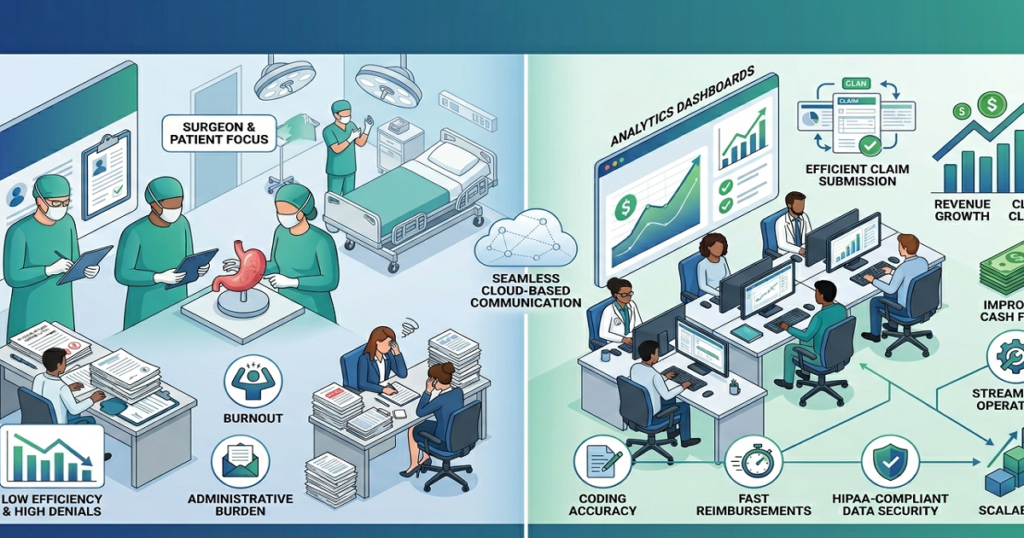
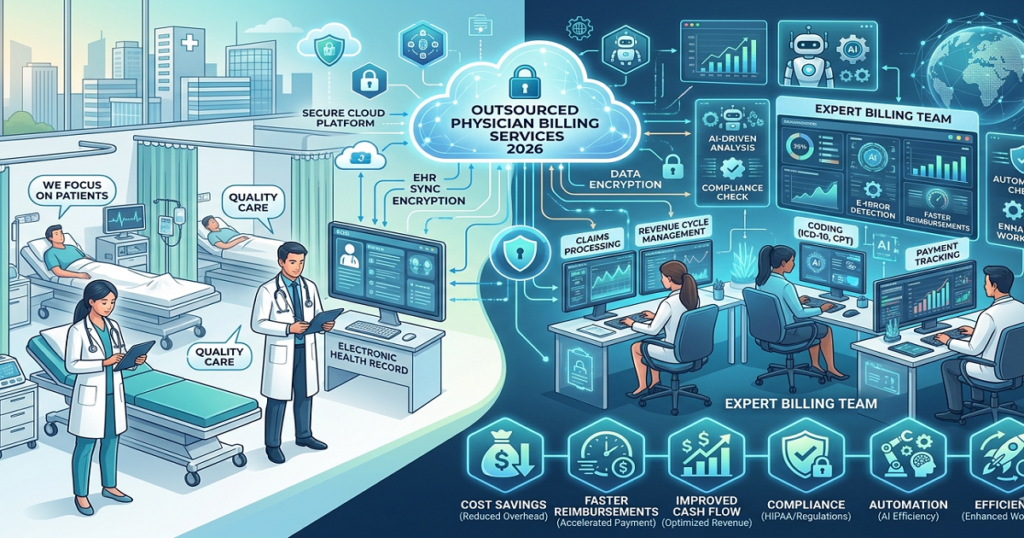
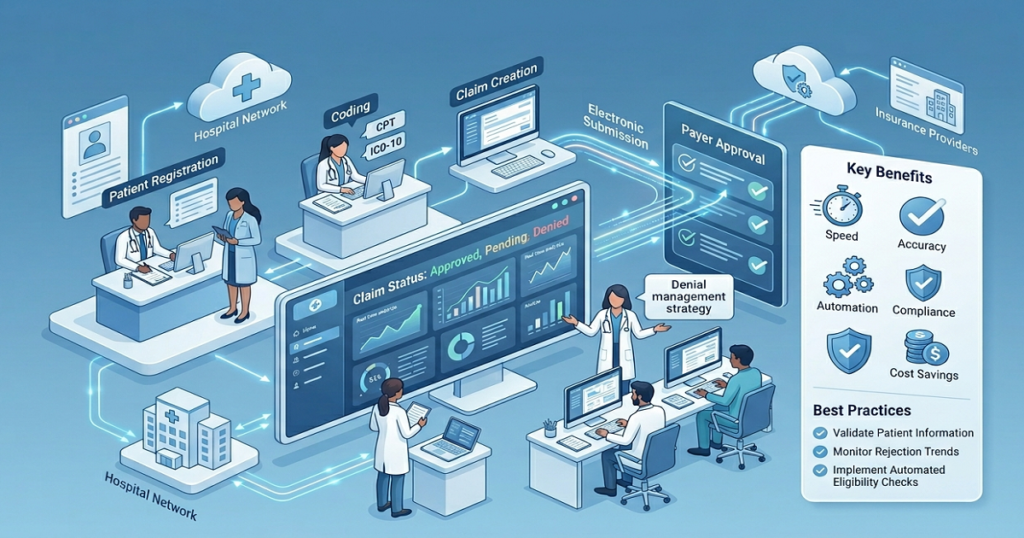
The Biggest Laboratory Revenue Cycle Challenges Labs Face Today
Medical BillingA lot of laboratories are dealing with slower reimbursements, even when testing volume stays high. Claims are getting submitted on time, but payments still take longer to arrive. Insurance companies request additional records more frequently, denied claims continue increasing, and billing teams spend more time correcting problems that could have been avoided earlier in the process. For many labs, the issue is not the number of tests being performed. The real problem is how difficult laboratory billing has become over the last few years. Payer rules change often. Medical necessity reviews have become stricter. Some insurance companies now require more supporting documentation before processing reimbursement, even for routine diagnostic testing. That is one reason laboratory revenue cycle challenges continue affecting labs across the country in 2026. Medical Necessity Reviews Are Delaying More Claims One of the biggest reimbursement problems laboratories deal with today involves medical necessity documentation. Insurance companies want to see that the diagnosis code supports the test being billed. If the diagnosis does not meet payer guidelines, the claim may come back denied or move into manual review. This happens more often with specialized or recurring testing. In many cases, the laboratory performs the testing correctly, but reimbursement still gets delayed because the documentation from the ordering provider does not fully support the payer’s requirements. That creates additional work later for billing teams trying to recover payment after the denial has already happened. Coding Problems Continue Slowing Down Reimbursements Laboratory billing depends heavily on coding accuracy. A small coding issue can delay payment much longer than many providers expect. This is especially common when: Most laboratories process a large number of claims daily, so even small coding inconsistencies can create larger reimbursement problems over time. Once denied claims begin increasing, billing teams spend more time fixing older accounts instead of focusing on current claim submissions. Common Signs Laboratory Billing Problems Are Growing Most labs do not notice a major billing problem all at once. It usually starts with smaller issues that keep repeating in the background. Claims stay unpaid longer than they should. Insurance companies keep asking for corrected documentation. Denials tied to diagnosis codes start showing up more often, and billing staff spend a large part of the day reopening old claims instead of working on current ones. As those unpaid claims continue sitting unresolved, accounts receivable start increasing, and payment flow becomes much less stable month to month. Billing Problem What It Usually Causes Incorrect diagnosis coding Claim denials Missing medical necessity support Payment delays Eligibility verification errors Rejected claims Delayed payer follow-up Aging unpaid balances Staff overload Billing backlogs Insurance Verification Creates Problems Earlier Than Most Labs Expect A lot of laboratory claims run into trouble because insurance details were not checked carefully before the test was billed. Some tests need prior authorization, while others have payer limits based on diagnosis codes or how frequently the patient can receive the test. If those requirements are missed upfront, the claim may stay unpaid or come back denied later. Many laboratories depend on insurance information provided by physician offices or patient registration systems. When coverage information is missing or inaccurate, the problem often does not appear until the insurance company rejects the claim later. As a result, billing staff spend more time going back to unresolved older claims instead of keeping up with current submissions and payer follow-ups. Payer Requirements Keep Changing One reason laboratory billing feels harder now is that insurance companies continue changing their reimbursement requirements. Different payers may apply different rules for: A claim that processes normally with one insurance company may still come back denied by another payer for the exact same service. That inconsistency creates ongoing billing pressure, especially for laboratories handling high claim volume across multiple insurance plans. This has become one of the larger laboratory revenue cycle challenges many labs are dealing with today. Insurance Follow-Up Takes More Time Than Before Submitting the claim is only one part of laboratory billing. A large amount of reimbursement work happens after submission. Insurance companies may request corrected claims, additional documentation, or clarification on medical necessity before payment is released. Some claims remain pending for weeks simply because nobody followed up consistently afterward. That process takes time every single day. Many laboratory billing teams are already managing: As workloads increase, follow-up delays become much more common. Once unresolved claims begin building up inside accounts receivable, collections usually start slowing down, too. Staffing Pressure Is Affecting Billing Workflows Many laboratories are operating with smaller administrative teams while billing workloads continue growing. When billing responsibilities are divided across a limited staff, even small delays become harder to control. Insurance follow-up may fall behind. Documentation corrections may stay unresolved longer than they should. Denied claims may not get reviewed quickly enough. The billing process gradually becomes harder to keep organized. Some laboratories do not realize how much revenue is tied up in unresolved claims until reimbursements become inconsistent month after month. Labs that monitor billing performance closely are usually able to identify these operational gaps earlier. Reporting Helps Labs Catch Problems Earlier A collections report by itself usually does not explain why payments are slowing down. Laboratories also need visibility into: Without that level of reporting, billing problems can continue quietly in the background for months before leadership notices the larger financial impact. Rapid RCM Solutions works with healthcare providers that need reliable billing support focused on cleaner claims, insurance follow-up, and reimbursement consistency. Final Thoughts Laboratory billing has become harder to manage as payer reviews, medical necessity requirements, and coding expectations continue to increase. For many labs, the challenge is no longer only submitting claims. The larger issue is keeping documentation accurate, verifying coverage correctly, and staying consistent with follow-up before unresolved claims begin affecting collections more seriously. That is why laboratory revenue cycle challenges continue affecting laboratories across the country. Labs that monitor denied claims closely, review payer trends regularly, and stay organized with billing follow-up are usually in a better position to
The Biggest Laboratory Revenue Cycle Challenges Labs Face Today Read More »