How Can Doctors Improve Patient Billing Without Hiring More Staff?
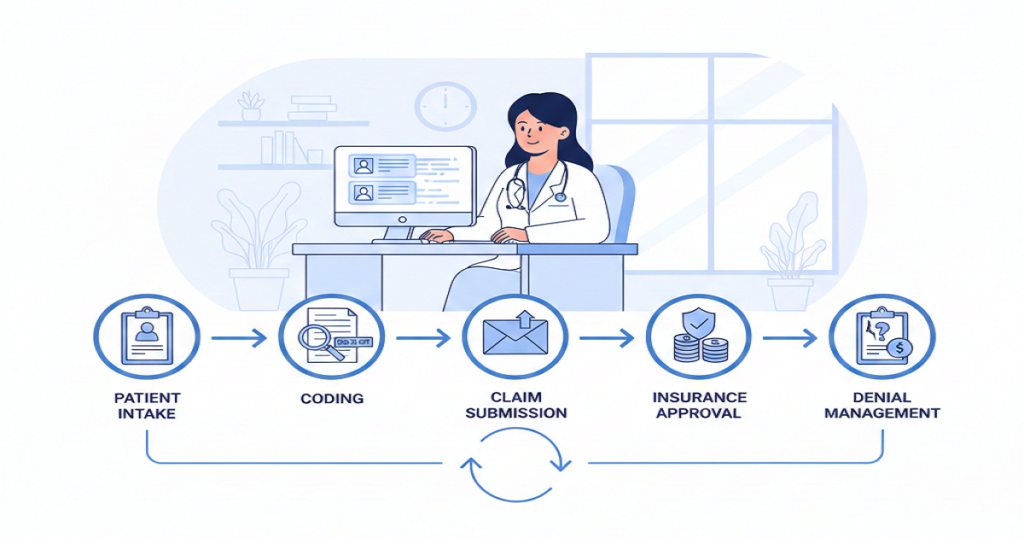
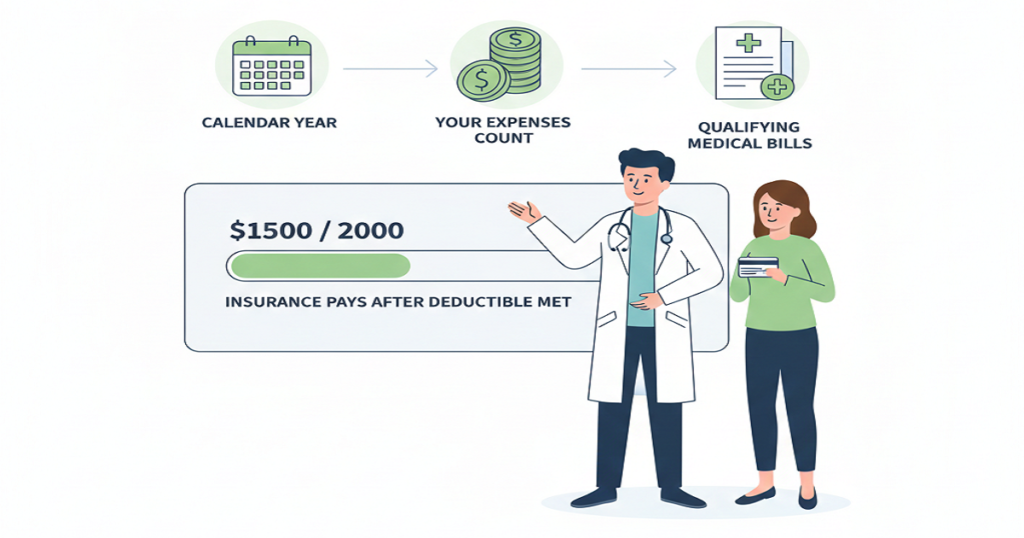
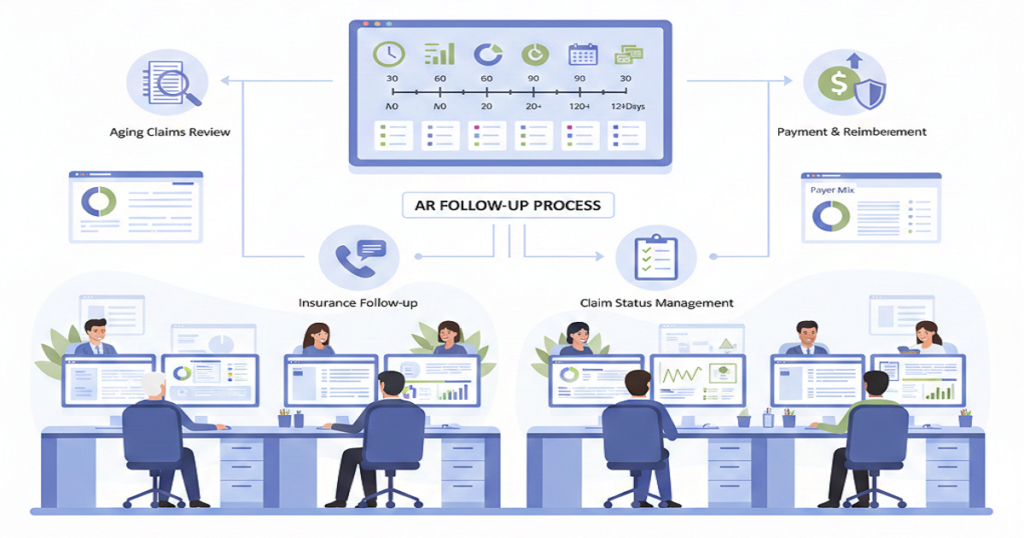
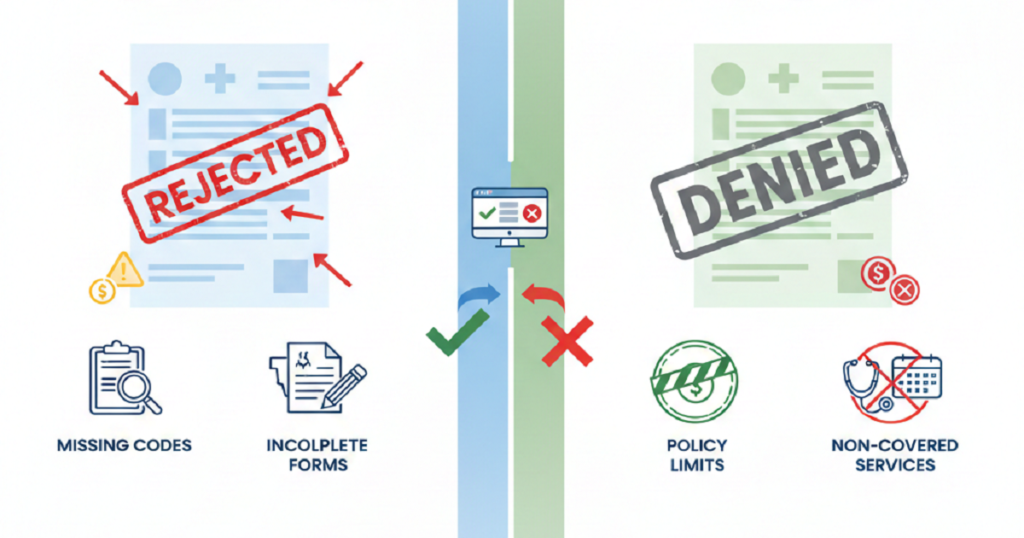
Medical BillingIf you ask any physician what’s been getting harder over the last few years, patient billing will be near the top of the list. More insurance rules, higher patient responsibility, slower payments, and the same-sized team trying to do twice the work. By the end of 2025, many practices realized they were spending more energy managing billing problems than practicing medicine. And yet, most of them weren’t in a position to keep hiring. Rising payroll, limited talent pools, and shrinking margins made that option unrealistic. So the real question for 2026 isn’t “who should we hire next?” It’s how doctors can improve patient billing with the team they already have. The good news is, this is completely achievable. And the practices that figure it out early gain a serious financial edge. Why Patient Billing Feels Broken Right Now Patient billing today is harder than it used to be for one simple reason: patients are paying more of the bill themselves. High-deductible plans, copays, coinsurance, and out-of-network charges now make up a large share of total collections. At the same time, payer processing is slower and more complex. That creates a dangerous gap between when care is delivered and when revenue actually arrives. The longer that gap grows, the more cash flow stress the practice feels. Hiring more staff doesn’t fix the root of the problem. Better systems do. Where Patient Billing Usually Breaks Down Before fixing anything, it helps to see what’s actually going wrong. The most common patient billing failures look like this: None of these requires new employees. They require better coordination. How Doctors Can Improve Patient Billing Using Smarter Workflows 1. Fix the Front Desk First Everything downstream depends on the accuracy of the first five minutes of a patient visit. Strong practices verify insurance at every visit, confirm deductibles and copays, and explain expected charges before the patient is seen. When this happens consistently, patient confusion drops and collections rise immediately. It also prevents a massive amount of rework later in the billing cycle. 2. Collect More at the Time of Service Waiting until after insurance processes the claim creates unnecessary risk. When practices collect copays, outstanding balances, and estimated patient responsibility before or during the visit, overall collection rates improve, and staff spend far less time chasing old balances. Clear communication here matters more than perfect numbers. Patients respond better when they know what to expect. 3. Submit Claims Faster and Cleaner The longer a claim sits, the less likely it is to be paid in full. Practices that submit clean claims within 24–48 hours of service consistently outperform those that wait. Clean claims reduce denials, speed reimbursement, and shorten the revenue cycle. This doesn’t require more staff. It requires better claim preparation and daily discipline. 4. Use Automation Where It Actually Helps Not all technology improves billing, but the right tools make a measurable difference. Automated eligibility checks, claim scrubbing, payment posting, and patient statement delivery remove repetitive work from staff and reduce errors. That gives your existing team more time to handle higher-value tasks like follow-ups and appeals. How to Improve Patient Communication Without Overloading Staff Patient billing often fails because patients don’t understand their bills. The solution isn’t more phone calls. It’s clearer communication. Modern practices use: When patients can see their balance, understand it, and pay it easily, collection rates rise without adding workload to the front office. Turn Denials Into a Billing Advantage Denials don’t just affect insurance revenue. They slow patient billing, too. Every delayed claim delays the patient statement. Every denied claim confuses the patient. Every appeal that drags on creates another billing problem. Practices that actively track denials, fix root causes, and resolve claims quickly shorten the entire billing cycle. That makes patient billing smoother and more predictable. Why Your Current Team Is Already Enough Most practices don’t suffer from a staffing shortage. They suffer from workflow chaos. When eligibility, documentation, coding, claims, patient billing, and follow-ups all operate in separate silos, even a large team feels overwhelmed. When those same functions run through a coordinated system, smaller teams outperform bigger ones. That’s the difference between working harder and working smarter. Where Rapid RCM Fits In Rapid RCM Solutions helps practices rebuild their billing operations without expanding headcount. Their model integrates eligibility verification, coding validation, clean claim submission, denial prevention, payment posting, patient billing, and follow-up into one continuous revenue workflow. The result is fewer errors, faster payments, stronger patient collections, and lower stress on internal staff. Practices using this model don’t just stabilize cash flow. They regain control of their business. What This Means for 2026 and Beyond Healthcare isn’t getting simpler. Patient responsibility will continue rising. Payer rules will keep tightening. And hiring will remain expensive. The practices that thrive in 2026 won’t be the ones with the biggest billing departments. They’ll be the ones with the smartest billing systems. Once doctors understand how doctors can improve patient billing through better workflows, technology, and communication, revenue becomes more predictable, operations become calmer, and growth becomes realistic again. Conclusion Improving patient billing doesn’t require hiring more people. It requires building better processes around the people you already have. When front-end verification improves, claims go out faster, denials shrink, patient communication becomes clearer, and collections become easier. The entire revenue cycle strengthens without adding headcount. For practices entering 2026, this shift isn’t optional anymore. It’s how stable growth is built. The doctors who master patient billing now will spend less time worrying about money later and more time focusing on care.
How Can Doctors Improve Patient Billing Without Hiring More Staff? Read More »